 Antibiotics | Anticancer drugs | Anticonvulsant / Seizure drugs | Benzodiazepines | NSAIDS | Thyroid drugs | Dermatology drugs | Lithium | Painkillers | Sex hormones | Asthma medications | Vaccines | High Blood Pressure drugs
Antibiotics | Anticancer drugs | Anticonvulsant / Seizure drugs | Benzodiazepines | NSAIDS | Thyroid drugs | Dermatology drugs | Lithium | Painkillers | Sex hormones | Asthma medications | Vaccines | High Blood Pressure drugs
Approximately 90 percent of all pregnant women use prescription or over-the-counter (OTC) medications at some point during their pregnancy. Experts contend that women should not use any OTC or prescription medications during pregnancy unless necessary for the health and welfare of the mother and/or child. Before becoming pregnant and during pregnancy, women should seek the early advice of their health care providers to discuss the use of OTC medications, prescription drugs, supplements, and vitamins.
Between two and ten percent of all birth defects are the direct result of using OTC or prescription medications during pregnancy.
How do drugs cause birth defects?
There are three ways that medications can cause birth defects:
- They can do direct damage to the fetus, causing abnormal development.
- They can compromise the function of the placenta, often by constricting blood vessels and reducing the supply of oxygen and nutrients from the mother to the fetus. This can lead to underdevelopment or low birth weight, which are risk factors for birth defects.
- They can trigger forceful uterine contractions, potentially injuring the fetus or prompting premature birth.
When is it most dangerous to take medications during pregnancy?
Depending on the medication, it may be dangerous to take certain medications at any point during pregnancy. However, research shows that a fetus is most vulnerable to teratogens (substances that cause birth defects) between the 3rd and 8th week after fertilization, when the organs and systems are developing. Certain drugs and other teratogens, however, can harm the fetus at any point during pregnancy. Teratogenic drugs taken before the 20th day following conception often have an all-or-nothing effect, inducing miscarriage or having no effect at all.
While drugs taken after the first trimester are less likely to result in serious birth defects, these teratogens can alter the function of organs and systems resulting in more subtle impairments and developmental defects.
How does the government regulate teratogenic drugs?
The Food and Drug Administration (FDA) uses a system of letters to classify drugs based on their teratogenic potential. Some drugs are highly toxic (classified with the letter ‘x’) and should never be used during pregnancy (i.e. thalidomide and Accutane). Other drugs, given ‘D’ classification are known to cause serious birth defects, but may be considered under certain conditions. The FDA’s ‘C’ category, where many drugs are classified, means that the risks to the fetus are unknown. Other drugs (in categories ‘A’ and ‘B’) are considered generally safe for use during pregnancy when taken for the welfare or health of the mother or child.
Alternative Drugs
In some cases, a drug may be used to replace another drug during pregnancy. For example, pregnant women with diabetes are often switched to insulin rather than oral hypoglycemic drugs (such as Chlorpropamide and Tolbutamide) because the former is less likely to harm the developing fetus. Heparin is often preferred for preventing blood clots, though it is known to increase the risk of osteoporosis and decrease a pregnant woman’s platelet count. Warfarin, its alternative, is known to cause serious birth defects. Propylthiouracil is preferred for hyperthyroidism. Sometimes certain anti-anxiety drugs and antibiotics are preferred over dangerous alternatives.
Dangers of Long-acting Medications
Certain drugs can pose a threat to a developing fetus long after the mother discontinues treatment. The drug etretinate, a drug in the same family as Accutane, is used to treat skin disorders. This dangerous drug is stored in subcutaneous fat and slowly released over long periods of time. The teratogenic effects of etretinate may still be present up to six months after terminating treatment. Many drugs can stay in the body for weeks after discontinuation, potentially affecting the fetus during this time.
Antibiotics
Certain drugs used to treat infections—antibiotics—can cause serious birth defects. While penicillins (i.e. amoxicillin and ampicillin), cephalosporins (i.e. cephalexin), and erythromycin are considered relatively safe during pregnancy, many types of antibiotics can cause serious harm to the fetus during pregnancy.
The following are antibiotics known or suspected to cause birth defects:
- Tetracycline (including minocycline, dixycycline, and oxytetracycline) can cause slowed bone growth, discoloration of the teeth, and increased vulnerability to cavities in the newborn. In some cases, the risk of liver failure can increase for women using this antibiotic during pregnancy.
- Sulfonamides (sulfa drugs) can cause jaundice and increase the risk of brain damage in a child, particularly when used during the third trimester of pregnancy. Can cause additional birth defects in women or fetuses with a G6PD* deficiency.
- Streptomycin (largely used to treat tuberculosis) can cause damage to the fetus’ ear, resulting in deafness.
- Nitrofurantoin can result in the breakdown of red blood cells in women or fetuses with a G6PD* deficiency.
- Kanamycin can cause ear damage, leading to deafness in the newborn.
- Ciprofloxacin has shown to cause joint abnormalities in animals.
- Chloramphenicol can cause Gray baby syndrome, a potentially fatal condition. Can also cause red blood cell breakdown in women or fetuses with a G6PD* deficiency.
- Trimethoprim blocks the action of folic acid, an important vitamin in the prevention of certain birth defects.
- Metronidazole is suspected by some experts to increase the risk of birth defects, though no definitive link has been established.
(*G6DP stands for glucose-6-phosphate dehydrogenase)
Anticancer drugs
Anti-cancer drugs work by stopping cancerous cells from multiplying in the patient, but when taken during pregnancy they can have extremely adverse effects on the development of the fetus. The chemotherapy drugs Busulfan, Chlorambucil, Cyclophosphamide, Mercaptopurine, Methotrexate can cause the following birth defects:
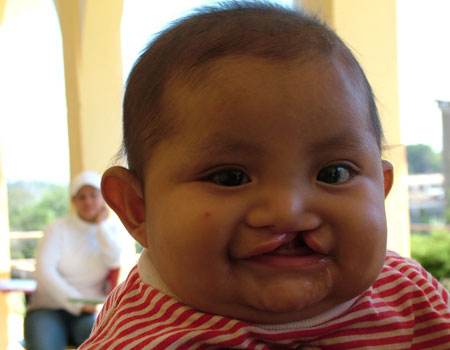 Underdevelopment of the fetus
Underdevelopment of the fetus- Underdevelopment of the lower jaw
- Cleft palate (Pictured at right)
- Abnormal development of the skull bones
- Clubfoot
- Spinal defects
- Ear defects
- Mental retardation
Drugs Vesanoid (tretinoin) and Targretin (bexarotene), both retinoids (see other retinoids below) can also increase the risks of birth defects.
Anticonvulsant/Seizure drugs
People with epilepsy often take these drugs for the control of seizures. Some of these medications can cause serious birth defects including mental retardation, spina bifida, deformed organs, cleft palate, and facial defects. According to a 2006 report in the Journal of Neurology, Neurosurgery, and Psychiatry, almost 96 percent of infants exposed to anti-eleptic drugs (AEDs) during development do not suffer birth defects; however, certain forms of AEDs pose a greater risk.
- Valproate (Depakote and Depakene) poses one of the greatest risks of birth defects. Combinations of AEDs containing valproate seem to pose a greater risk than AED combinations without valproate. This drug can increase the risk of cleft palate, and facial, skull, heart, and abdominal organ defects. Studies have shown the fetuses exposed to valproate during development are FOUR times more likely to suffer birth defects than fetuses not exposed to this anticonvulsant.
- Topiramate can increase the risk of oral cleft birth defects by nearly four times that of other antiepileptic drugs.
- Trimethadione can increase the risk of miscarriage.
- Phenytoin and Phenobarbitol can increase the risks of bleeding in the newborn and other birth defects
- Carbamazipine can also increase the risk of certain birth defects.
Benzodiazepines
Benzodiazepines, such as tranquilizers, anti-anxiety drugs, and sleeping pills, can cause trouble nursing in newborns and other complications. This class of drugs is known to increase the risk of newborn drug dependency, temperature problems, breathing difficulties, and muscle problems.
- Valium (diazepam), when taken late in pregnancy, can cause depression, irritability, exaggerated reflexes, shaking, and limpness (called Floppy baby syndrome) in the newborn.
- Chlordiazepoxide can also increase the risks of birth defects, particularly when used during the first trimester.
- Clonazepam, Lorazepam, and Temazepam have shown to cause birth defects in animal studies.
Non-steroidal Anti-inflammatory Drugs (NSAIDS)
Aspirin and other salicylates, particularly when used late in pregnancy, can increase the risk of low birth weight, delayed onset of labor, and possible death of the newborn. These medications can also increase the risk of jaundice, severe bleeding (in the fetus or mother), and the premature closing of the connection between the aorta and the artery to the lungs. Other analgesics, such as Codeine and hydrocodone, have shown to increase the risks of birth defects in animal studies. Use of narcotics during pregnancy can increase the risk of drug dependence and breathing problems in the newborn.
Ibuprofen (Advil and Motrin), Ketoprofen (Orudis), and Naproxen (Aleve) should be used with caution during pregnancy and be avoided completely during the third trimester to mitigate the risk of birth defects.
Accutane, retinoids, and other dermatology drugs
Accutane (isotretinoin) is a popular prescription drug approved to treat severe nodular acne in patients for whom other treatments have not been successful. However, this drug is commonly prescribed (arguably over-prescribed) to patients with mild to moderate acne. Accutane use during pregnancy poses an extremely high risk of birth defects or death. Even a small amount of this drug used for a short time poses serious risks. The risk is so great that the FDA requires a number of criteria be met before a female can receive a prescription for this medication.
Under the iPledge system, prior to receiving a prescription of Accutane, a patient must have two negative pregnancy tests, sign a consent form stating they understand the risk of birth defects posed by this drug, and agree to use two forms of birth control prior to, during, and after use of Accutane.
The possible birth defects caused by Accutane include:
- Mental retardation and learning disabilities
- Eye and ear deformities
- Cleft lip, cleft palate and other facial abnormalities
- Heart defects
- Microcephaly (small head and brain)
- Hydrocephaly (enlarged fluid-filled spaces within the brain)
Accutane also increases the risks of miscarriage, premature birth, and infant death.
Soriatane (acitretin), used to treat psoriasis, can cause spina bifida, craniofacial and heart defects, and limb defects. Soriatane stays in the body for a long time and should NOT be used by any woman planning to conceive for the next THREE YEARS after terminating treatment with this drug.
Tegison (etretinate), used to treat psoriasis, also stay in the body a long time. Some medical experts state that women who have used this dermatological treatment should avoid pregnancy for an indefinite period of time, due to the serious risk of birth defects.
Topical retinoids, commonly used to treat acne and sun-damaged skin, are suspected to cause birth defects, though the risks are unknown and unproven. These medications include Retin-A, Renova, Differen, and Tazorac.
Vitamin A, belonging to the same family as these retinoids, can also cause birth defects when taken in high doses. While Vitamin A is essential to normal fetal development, doses in excess of 10,000 IU (international units) daily (two times the amount recommended by the FDA) can increase the risks of serious birth defects. You may wish to speak with your health care provider about safe levels of Vitamin A—as well as other vitamins, minerals, and supplements—during pregnancy.
Antidepressants
 Paxil (paroxetine) is a popular anti-depressant medication approved to treat depression and other psychiatric disorders. In 2005, the FDA issued a health advisory warning consumers that taking Paxil during the first trimester of pregnancy nearly doubles the risk of delivering a child with heart defects (atrial and ventricular septal defects). Women who are pregnant or plan to become pregnant should speak with their doctors prior to initiating, changing, or terminating treatment with Paxil.
Paxil (paroxetine) is a popular anti-depressant medication approved to treat depression and other psychiatric disorders. In 2005, the FDA issued a health advisory warning consumers that taking Paxil during the first trimester of pregnancy nearly doubles the risk of delivering a child with heart defects (atrial and ventricular septal defects). Women who are pregnant or plan to become pregnant should speak with their doctors prior to initiating, changing, or terminating treatment with Paxil.
Prozac (fluoxetine) is another top-selling anti-depressant medication associated with an increase in serious birth defects. A study published in the New England Journal of Medicine (February 9, 2006) shows that Prozac use during the third trimester of pregnancy more than doubles the risk of delivering a child with PPHN, or persistent pulmonary hypertension of the newborn.
PPHN is a rare but potentially fatal condition whereby the baby’s respiratory system does not properly adapt to breathing in the outside world. Despite treatment, ten to twenty percent of all babies with PPHN do not survive.
Prozac has also shown to increase the risks of other neonatal complications including jitteriness, hypotonia, and breathing problems.
Some studies have associated use of the drug Zoloft (sertraline) and other SSRIs (selective serotonin reuptake inhibitors) with an increased risk of birth defects.
Painkillers
OxyContin increases the risk of serious birth defects such as congenital heart defects, spina bifida, hydrocephaly, congenital glaucoma and gastroschisis. Risk of hypoplastic left heart syndrome is doubled for women who take OxyContin just before or during pregnancy.
Thyroid Drugs
The thyroid drugs, Methimazole, Propylthiouracil, and radioactive iodine, can increase the risks that a child will be born with an under-active, over-active, or enlarged thyroid gland.
Fertility Drugs
Clomid is a fertility drug that belongs to a category called ovulatory stimulants. Use of Clomid just before or during pregnancy is linked to many serious birth defects, including but not limited to Down’s syndrome, club foot, oral clefts, anencephaly (open cranium with the absence of brain), esophageal atresia (closed esophagus), three types of heart defects and many more issues.
Sex Hormones
Sex hormones are commonly used to treat certain blood and other conditions. These drugs can increase the risk of birth defects.
- Danazol can cause a masculinization of a female child’s genitals. In some cases, surgery is necessary to treat this serious birth defect.
- Diethylstilbestrol (DES) use can result in menstrual problems, abnormalities of the uterus, an increased risk of vaginal cancer, and pregnancy complications in daughters; can lead to penis abnormalities in sons.
- Estrogens (Premarin) and synthetic progestins (not the low doses found in oral contraceptives) can also increase the risks of birth defects. Premarin, in the FDA’s category X, is known to cause serious birth defects.
Thalidomide
Thalidomide is a drug approved by the FDA to treat leprosy. This drug is known to pose a very high risk of serious birth defects. Even taking a single dose of thalidomide during pregnancy can result in serious birth defects. In the late 1950s, thalidomide was used to treat anxiety, insomnia, and even morning sickness in expecting mothers. It was taken off the market in the 1960s, after more than 10,000 children, whose mothers used thalidomide, were born with serious malformations, missing limbs, and other serious side effects.
In 1998, the FDA approved this drug for the treatment of erythema nodosum leprosum (ENL), a complication of leprosy, despite irrefutable evidence that this drug poses serious birth defect risks. Studies have shown that two-thirds of all women of childbearing age are unaware of the serious risks associated with taking thalidomide during pregnancy.
Vaccines
 Live-virus vaccines—including those used to prevent measles, mumps, German measles (Rubella), polio, chicken pox, and yellow fever—can increase the risk of birth defects. A woman who has received a measles-mumps-rubella (MMR) vaccine or a vaccination against chickenpox should not get pregnant for at least one month after treatment. The rubella vaccine is known to cause placental and fetal infection. If a woman is in danger of contracting cholera, typhoid, polio, or hepatitis A or B, the use of vaccinations may be considered, though not recommended, during pregnancy.
Live-virus vaccines—including those used to prevent measles, mumps, German measles (Rubella), polio, chicken pox, and yellow fever—can increase the risk of birth defects. A woman who has received a measles-mumps-rubella (MMR) vaccine or a vaccination against chickenpox should not get pregnant for at least one month after treatment. The rubella vaccine is known to cause placental and fetal infection. If a woman is in danger of contracting cholera, typhoid, polio, or hepatitis A or B, the use of vaccinations may be considered, though not recommended, during pregnancy.
Lithium
Lithium is a mood-stabilizing drug known to cause structural heart and other defects, low muscle tone, lethargy, under-active thyroid gland, poor feeding, and a condition called nephrogenic diabetes insipidus in the newborn.
High Blood Pressure Drugs
ACE Inhibitors (Angiotensin-converting enzyme Inhibitors) also called antihypertensives, when taken late in pregnancy, can increase the risk of fetal kidney damage, low amniotic fluid, and structural defects of the face, lungs, and limbs.
Thiazide diuretics can lower levels of oxygen, potassium, and platelets in the fetus’s blood.
Asthma Medications
Studies regarding the safety of asthma medications during pregnancy are conflicting and limited at best. Some studies have shown a positive relationship between first trimester use of corticosteroids and structural birth defects and Down syndrome. However, many studies confirm the non-teratogenity of corticosteroids. Other findings support the link between these drugs and preclampsia, low birth weight, and premature birth.
Because studies regarding asthma medication use during pregnancy are very limited, it is important to speak with a doctor to weigh the risks of benefits of using asthma medications during pregnancy. Most experts recommend a conservative approach to treating asthma with medication while pregnant.
Not all over-the-counter, prescription, and alternative medications have been tested for their effects on fetal development. For ethical reasons, most drug makers avoid testing women of childbearing age, who may be pregnant, when determining the effects of their products. Therefore, it is important to exercise extreme caution when using any form of medication during pregnancy. Before starting, stopping, or changing medications, it is always wise to speak with a qualified health care provider to weigh the risks and benefits of your particular treatment.
Has your prescription drug use resulted in birth defects?
If you took a teratogenic medication during pregnancy, which caused birth defects in your child, you may be eligible to seek compensation for your past and future medical bills, expenses, pain and suffering, and more. Please contact the experienced attorneys at The Oshman Firm today for a FREE consultation of your case. We are prepared to protect the best interests of you and your family.
